People with one of the type A blood groups are more likely to have a stroke before the age of 60 compared with people with other blood types, research shows.
Blood types describe the rich variety of chemicals displayed on the surface of our red blood cells.
Among the most familiar are those named A and B, which can be present together as AB, individually as A or B, or not present at all, as O.
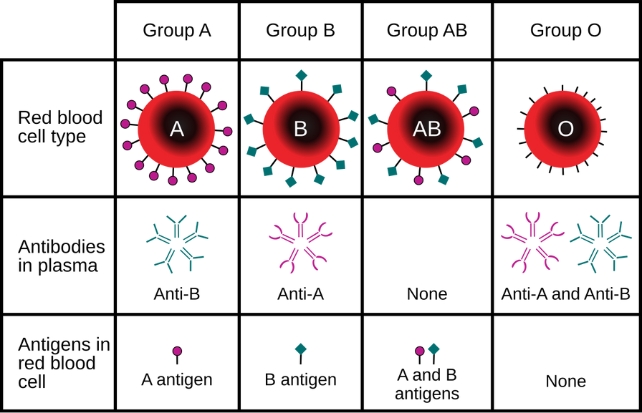
Even within these major blood types, there are subtle variations arising from mutations in the genes responsible.
In a study published in 2022, genomics researchers uncovered a clear relationship between the gene for the A1 subgroup and early onset stroke.
Researchers compiled data from 48 genetic studies, which included roughly 17,000 people with a stroke and nearly 600,000 non-stroke controls. All participants were between 18 and 59 years of age.
A genome-wide search revealed two locations strongly associated with an earlier risk of stroke. One coincided with the spot where genes for blood type sit.
A second analysis of specific types of blood-type gene then found people whose genome coded for a variation of the A group had a 16 percent higher chance of a stroke before the age 60, compared with a population of other blood types.
For those with a gene for group O1, the risk was lower by 12 percent.
The researchers noted, however, that the additional risk of stroke in people with type A blood is small, so there is no need for extra vigilance or screening in this group.
“We still don’t know why blood type A would confer a higher risk,” said senior author and vascular neurologist Steven Kittner from the University of Maryland.
“But it likely has something to do with blood-clotting factors like platelets and cells that line the blood vessels as well as other circulating proteins, all of which play a role in the development of blood clots.”
While the study findings may seem alarming – that blood type could change early stroke risk – let’s put these results into context.
Each year in the US just under 800,000 individuals experience a stroke. Most of these events – around three out of every four – occur in people 65 years and older, with risks doubling every decade after the age of 55.
Also, the people included in the study lived in North America, Europe, Japan, Pakistan, and Australia, with people of non-European ancestry only making up 35 percent of participants. Future studies with a more diverse sample could help clarify the significance of the results.
“We clearly need more follow-up studies to clarify the mechanisms of increased stroke risk,” Kittner said.
Another key finding of the study came from comparing people who had a stroke before the age of 60 to those that had a stroke after the age of 60.
For this, the researchers used a dataset of about 9,300 people over the age of 60 who had a stroke, and some 25,000 controls over the age of 60 who didn’t have a stroke.
They found that the increased risk of stroke in the type A blood group became insignificant in the late-onset stroke group, suggesting that strokes that happen early in life may have a different mechanism compared to those that occur later on.
frameborder=”0″ allow=”accelerometer; autoplay; clipboard-write; encrypted-media; gyroscope; picture-in-picture; web-share” referrerpolicy=”strict-origin-when-cross-origin” allowfullscreen>
Strokes in younger people are less likely to be caused by a build-up of fatty deposits in the arteries (a process called atherosclerosis) and more likely to be caused by factors to do with clot formation, the authors said.
The study also found that people with type B blood were around 11 percent more likely to have a stroke compared to non-stroke controls regardless of their age.
Previous studies suggest that the part of the genome that codes for blood type, called the ‘ABO locus’, is associated with coronary artery calcification, which restricts blood flow, and heart attack.
The genetic sequence for A and B blood types have also been associated with a slightly higher risk of blood clots in veins, called venous thrombosis.
This paper was published in Neurology.
An earlier version of this article was published in September 2022.











Leave a Reply